19 Chapter 19 – Trauma, Therapy, and Trauma Informed Care
Ericka Goerling, PhD and Emerson Wolfe, MS
Learning Outcomes
- Demonstrate an understanding of the issues involved in sexual violence (rape, child sexual abuse, and sexual harassment) including factors that may contribute to these types of violence; characteristics of offenders, treatment resources and prevention strategies.
- Differentiate between human trafficking and sex work.
- Examine the impact of sexual trauma on individuals and discuss trauma-informed clinical practices.
Introduction

At the outset of this particular section, we want to note that since we are discussing issues associated with sexual violence, this chapter may be difficult. It will be especially important, if you are a survivor of assault yourself, if you love a survivor, or if you deeply feel the inherent injustices of gendered and/or sexual violence, that you take good care of yourself during this section’s reading and discussions (take lots of breaks, remember to prioritize hydration, good food, and sleep, talk to a friend/loved one if you need to, exercise, random dance parties, or gentle care of your body are all useful).
This section will identify, though an historical lens, the development of rape culture. We seek to define and give rates of various forms of sexual violence, as well as offer important, emerging practices of response to survivors. As always, we view the complex issues of sexual trauma through an intersectional lens.
Definitions: Rape Culture and Types of Sexual Violence
Rape Culture
In a society ruled by rape culture, women and gender minorities are told to protect themselves from the wrath of cisgender men because they cannot control themselves in regards to their sexual gratification needs and their unrelenting anger. Violence in this system is normalized and justified with those harmed being blamed for not taking enough precautions to prevent the attack from occurring. Not only is this harmful to women and other gender minorities, but men are also harmed when they are perceived as too feminine or gay. Only the most masculine, absent of empathy, prevail in this broken culture.
The criminal justice system is devoid of true justice when recourse is provided to a select few who jump through the endless emotional and retraumatizing hoops to finally have their voices heard and validated in court. Systems work to protect perpetrators, whether that be through the backlog of untested rape kits in storage at police departments to the people around those in power who support or do nothing to stop sexual harassment and abuse from occurring (the Catholic Church, the Boy Scouts of America, Harvey Weinstein and Hollywood, and so many more). “A rape culture is one that tolerates and even glorifies male sexual aggression against women” including these additional elements: “rape myth acceptance (Lee, Kim, & Lim, 2010; Suarez & Gadalla, 2010), ambivalent sexism (Chapleau, Oswald, & Russell, 2007; Masser, Lee, & McKimmie, 2010), victim blaming (Abrams, Viki, Masser, & Bohner, 2003; Sleath & Bull, 2012), and normalization of sexual violence (i.e., a sense that sexual violence and assault is inevitable and ubiquitous; Hlavka, 2014)” (as cited in Klement et al., 2017, p. 131).
Sexual Violence: Definition, Tactics, and the Law
Sexual violence is when a sexual act is carried out or attempted against someone who does not freely consent, cannot consent or cannot refuse; may also involve coercing the victim to engage in sexual acts with other people, animals or objects (Basile et al., 2014).
Basile et al. (2014) elaborates further on the terms related to consent or lack of consent and their exact definitions are provided:
- Consent
Words or overt actions by a person who is legally or functionally competent to give informed approval,
indicating a freely given agreement to have sexual intercourse or sexual contact. - Inability to Consent
A freely given agreement to have sexual intercourse or sexual contact could not occur because of the
victim’s age, illness, mental or physical disability, being asleep or unconscious, or being too intoxicated
(e.g., incapacitation, lack of consciousness, or lack of awareness) through their voluntary or involuntary
use of alcohol or drugs. - Inability to Refuse
Disagreement to engage in a sexual act was precluded because of the use or possession of guns or
other non-bodily weapons, or due to physical violence, threats of physical violence, intimidation or
pressure, or misuse of authority. (p. 11)
Sexual harassment, sexual assault, sexual abuse, rape, incest, child sexual abuse, and sex trafficking are all forms of sexual violence.
How do we define sexual harassment? The difficulty here is that it is often based on individual perceptions of comments which can be difficult to prove without witnesses or others who have experienced similar experiences of sexual harassment. The term “social-sexual behavior” has been developed “in order to include behaviors that potentially could be perceived as sexual harassment and that contains sexual elements such as impersonal, derogatory jokes, unwanted dating requests, or physical contact” (Kessler et al., 2019, p. 1272). Perception of these social-sexual behaviors is dependent upon individual factors (experiences, values, attitudes, etc.) and contextual factors (relationship type and situation) (Kessler et al., 2019).
Tactics
Perpetrators of sexual violence and human sex trafficking may use the following tactics against those in which they seek to sexually harm:
- use or threat of physical harm
- providing alcohol or substances to gain compliance
- taking advantage of someone who voluntarily became intoxicated and cannot consent
- exploitation of vulnerabilities (exploiting someone based on their intersecting marginalized identities, such as an undocumented immigration status, threats of outing someone for their undisclosed sexual orientation or gender identity, disability, age, etc.)
- intimidation
- misuse of authority
- economic coercion (promise of money, housing and other resources)
- degradation through increasingly demeaning comments and treatment
- fraud (pretending to be someone they are not)
- continued verbal pressure
- false promises by the perpetrator (promising resources they don’t actually have, promise of marriage or a relationship, etc.)
- emotionally manipulative threats (i.e. threat to spread rumors)
- grooming to gain trust
- threats to control someone’s sexual behavior (pregnancy, STIs, etc.) (Basile et al., 2014)
Profile of Someone Who Harms Others
This information was taken from the Center for Disease Control and Prevention (CDC) (2020)
- We all have the capacity to hurt others or be hurt by someone else
- All gender identities, sexual orientations, ages, etc.
- The perpetrator is usually someone known to the victim
- Most commonly a cisgender, straight male
Click on this resource for more information on the CDC’s Violence Prevention programs.
Legal Definitions
According to the United States Department of Justice (2020), “the term ‘sexual assault’ means any nonconsensual sexual act proscribed by Federal, tribal, or State law, including when the victim lacks capacity to consent.”
Sexual harassment in the workplace is divided under US law into two categories (Kessler et al., 2019):
- quid pro quo harassment (employment advancements contingent upon sexual conduct)
- hostile work environment type harassment (such as sexism or homonegativity)
Check out PCC’s information on Sexual Harassment and Misconduct which includes definitions for sexual harassment and misconduct as well as information on your rights, how to seek help, and how to file a report.
Historical Origins and Current Times
Ancient Beginnings: Colonialism, War, and Sexual Violence
Rape culture connects with colonialism through warfare and sexual violence toward communities who are caught along the warpath. Writings, images, and art depicting sexual violence during war by Israelites, Greeks and Romans have been uncovered by archaeologists and historians (Vikman, 2005).
Israelites: Rape and sexual violence are condoned during wartime in the Old Testament (Deuteronomy, Numbers, and more).
Greeks: Homer’s the Iliad has many rape scenarios and normalizes this as part of the chaos and plundering of war. Homer begins to explore sexual violence from the lens of disgust and morality while at the same time women are described as lesser than men and making men seem more feminine is meant to insult masculinity.
Romans: Boys and men were also depicted as being sexually violated by out-of-control soldiers unable to be controlled by their commanders–kill first then plunder the city and rape the people. The Romans were particularly brutal in how they sexually terrorized the communities they attacked.
Common themes: revenge, anger, power, subjugation, sexual gratification, making enemies more pure by passing on their line through them impregnating the women, breakdown of social order, and chaos (Vikman, 2005).
#MeToo Movement and Changing Norms
As the harms of rape culture are being discussed more openly through the #MeToo movement and social outcry is increasing against those who are accused of sexual misconduct and sexual violence, a culture of consent is gaining traction and support (Kessler et al., 2019).
Check out this article from Klement et al. (2017) titled, “Participating in a Culture of Consent May Be Associated With Lower Rape-Supportive Beliefs” for more information on research being conducted on this concept.
The Oregon Department of Education has created these lesson plans to teach consent to students in elementary school in an age and developmentally appropriate way:
- K-2 My Space, Your Space Lesson (Online/Offline Adaptation)
- K-2 Seeking Help Lesson (Online/Offline Adaptation)
- K-2 Understanding Our Bodies: The Basics Lesson (Online/Offline Adaptation)
- 3-5 Your Body, Your Rights Lesson (Online/Offline Adaptation)
- Grade 5 Sexual and Reproductive Anatomy Lesson (Online/Offline Adaptation)
Risk and Protective Factors
The following information in this section is taken directly from the CDC (2020) in regards to risk and protective factors for sexual violence.
Risk Factors for Perpetration
Individual Risk Factors
- Alcohol and drug use
- Delinquency
- Lack of concern for others
- Aggressive behaviors and acceptance of violent behaviors
- Early sexual initiation
- Coercive sexual fantasies
- Preference for impersonal sex and sexual-risk taking
- Exposure to sexually explicit media
- Hostility towards women
- Adherence to traditional gender role norms
- Hyper-masculinity
- Suicidal behavior
- Prior sexual victimization or perpetration
Relationship Factors
- Family history of conflict and violence
- Childhood history of physical, sexual, or emotional abuse
- Emotionally unsupportive family environment
- Poor parent-child relationships, particularly with fathers
- Association with sexually aggressive, hypermasculine, and delinquent peers
- Involvement in a violent or abusive intimate relationship
Community Factors
- Poverty
- Lack of employment opportunities
- Lack of institutional support from police and judicial system
- General tolerance of sexual violence within the community
- Weak community sanctions against sexual violence perpetrators
Societal Factors
- Societal norms that support sexual violence
- Societal norms that support male superiority and sexual entitlement
- Societal norms that maintain women’s inferiority and sexual submissiveness
- Weak laws and policies related to sexual violence and gender equity
- High levels of crime and other forms of violence
Protective Factors for Perpetration
Protective factors may lessen the likelihood of sexual violence victimization or perpetration. These factors can exist at individual, relational, community, and societal levels.
- Families where caregivers work through conflicts peacefully
- Emotional health and connectedness
- Academic achievement
- Empathy and concern for how one’s actions affect others
Rates and Statistics
According to the CDC’s (2021) information on Preventing Sexual Violence:
- 1 in 3 women and 1 in 4 men experienced sexual violence involving physical contact during their lifetimes. Nearly 1 in 5 women and 1 in 38 men have experienced completed or attempted rape and 1 in 14 men was made to penetrate someone (completed or attempted) during his lifetime.
- 1 in 3 female rape victims experienced it for the first time between 11-17 years old and 1 in 8 reported that it occurred before age 10. Nearly 1 in 4 male rape victims experienced it for the first time between 11-17 years old and about 1 in 4 reported that it occurred before age 10.
- Sexual violence is costly. Recent estimates put the cost of rape at $122,461 per victim, including medical costs, lost productivity, criminal justice activities, and other costs.
Here are some more statistics from RAINN (2020) titled, “Victims of Sexual Violence: Statistics.”
Since many statistics leave out transgender individuals, here is a resource that specifically focuses on the impact of sexual assault on transgender individuals from the Office for Victims of Crime.
Human Sex Trafficking
Sex work is consensual whereas prostitution and engaging in sexual acts as a result of being human trafficked is not at all consensual no matter the degree to which the individual is bought into this way of life. Immense psychological suffering and psychological manipulation tactics are used by perpetrators to lock in people in a way that makes them feel or believe that engaging in prostitution or other sex acts is the only way to survive. Perpetrators seek out people who have marginalized intersecting identities and use their power to control and coerce them.
Sexual trafficking is legally defined by Basile et al. (2014) as “the recruitment, harboring, transportation, provision, or obtaining of a person for the purpose of a commercial sex act. In order for a situation to be considered trafficking, it must have at least one of the elements within each of the three criteria of process, means, and goal. If one condition from each criterion is met, the result is trafficking. For adults, victim consent is irrelevant if one of the means is employed. For children, consent is irrelevant with or without the means category.
- Process: Recruitment, transportation, transferring, harboring, or receiving.
- Means: Threat, coercion, abduction, fraud, deceit, deception, or abuse of power.
- Goal: Prostitution, pornography, violence/sexual exploitation, or involuntary sexual servitude” (p. 16).
Read this dissertation titled, “From the Voices of Domestic Sex Trafficking Survivors: Experiences of Complex Trauma & Posttraumatic Growth,” by Evans (2019).
Trauma Responses and Impacts: PTSD Explained
Trauma: In this text, the term “trauma” refers to experiences that cause intense physical and psychological stress reactions. It can refer to “a single event, multiple events, or a set of circumstances that is experienced by an individual as physically and emotionally harmful or threatening and that has lasting adverse effects on the individual’s physical, social, emotional, or spiritual wellbeing” (SAMHSA, 2012, p. 2). Trauma can affect people of every race, ethnicity, age, sexual orientation, gender, psychosocial background, and geographic region. A traumatic experience can be a single event, a series of events, and/or a chronic condition (e.g., childhood neglect, domestic violence). Traumas can affect individuals, families, groups, communities, specific cultures, and generations. It generally overwhelms an individual’s or community’s resources to cope, and it often ignites the “fight, flight, or freeze” reaction at the time of the event(s). It frequently produces a sense of fear, vulnerability, and helplessness.
It is not just the event itself that determines whether something is traumatic, but also the individual’s experience of the event. Two people may be exposed to the same event or series of events but experience and interpret these events in vastly different ways. Various biopsychosocial and cultural factors influence an individual’s immediate response and longterm reactions to trauma. For most, regardless of the severity of the trauma, the immediate or enduring effects of trauma are met with resilience—the ability to rise above the circumstances or to meet the challenges with fortitude.
For some people, reactions to a traumatic event are temporary, whereas others have prolonged reactions that move from acute symptoms to more severe, prolonged, or enduring mental health consequences (e.g., posttraumatic stress and other anxiety disorders, substance use and mood disorders) and medical problems (e.g., arthritis, headaches, chronic pain). Others do not meet established criteria for posttraumatic stress or other mental disorders but encounter significant trauma-related symptoms or culturally expressed symptoms of trauma (e.g., somatization, in which psychological stress is expressed through physical concerns). For that reason, even if an individual does not meet diagnostic criteria for trauma-related disorders, it is important to recognize that trauma may still affect his or her life in significant ways. For the full diagnostic criteria of posttraumatic stress disorder, click HERE.
Distinctive Characteristics for Sexual Assault Survivors
It’s important to consider that the experience and aftermath of a traumatic event are influenced by social identity factors such as age, race, class, sexual orientation, disability, and gender (Richmond, Geiger, & Reed, 2013). Particularly in cases of sexual assault, practitioners must confront the pervasive societal messages that unnecessarily blame victims and minimize the experience of rape/incest (Ryan, 2011; as cited in Richmond, Geiger, & Reed, 2013). These messages can become internalized, resulting in self-defeating thoughts and powerful emotions, such as shame and guilt. Unfortunately, it’s not uncommon for survivors of sexual trauma to describe themselves in terms of self-loathing and intense vulnerability, which can undermine resiliency and growth (Lewis, Robillard, Billings, & White, 2019). For this reason, most trauma therapies recognize that attention to a survivor’s identity, as well as social constructs as critical to the healing process (Richmond, Geiger, & Reed, 2013).
Often, shame distorts sexual assault survivor’s perception of responsibility for the trauma. Some survivors, especially those who have kept the trauma secret, may not receive needed comfort and acceptance from others; they are also are more likely to struggle with issues of causation (e.g., feeling responsible for the sexual assault), to feel isolated by the trauma, and to experience repeated trauma that makes them feel victimized (Center for Substance Abuse Treatment, 2014). In cases in which the survivor knows their assailant, issues of victim-blaming may be more pronounced. Yet, several studies have demonstrated that survivors of known offenders are as likely to develop symptoms of trauma as victims of stranger sexual assault (Lewis, et al., 2019).
Sexual violence is often traumatic, and experiencing it can affect how the brain and body work together. During any traumatic event, the body goes into crisis mode and processes memories and reactions very differently. The brain releases chemicals that control how a person will react to the event and alter how a survivor experiences and/or remembers the violence that happened. How a person reacts is not a conscious choice, survivors can experience automatic reflexes that make them immobile and unable to fight or flee (Wilson, Lonsway, Archambault, & Hopper, 2016; as cited in Benner, 2018, p. 32). When a danger or threat is detected, different defense states emerge including hypervigilance (freeze-alert), fight or flight, tonic immobility (freeze-fright), and collapse (for more on the specifics to these mechanism, see Cuevas, et al., 2018)
For one of the best narrations on the topic of trauma’s impact on the body, check out the On Being interview between psychiatrist Bessel van der Kolk and Krista Tippett (not required but a useful resource).
Trauma Recovery (Trauma Informed Care & Evidenced Based Interventions)
Trauma-informed: A trauma-informed approach to the delivery of behavioral health services includes an understanding of trauma and an awareness of the impact it can have across settings, services, and populations. It involves viewing trauma through an ecological and cultural lens and recognizing that context plays a significant role in how individuals perceive and process traumatic events, whether acute or chronic. In May 2012, SAMHSA convened a group of national experts who identified three key elements of a trauma-informed approach: “(1) realizing the prevalence of trauma; (2) recognizing how trauma affects all individuals involved with the program, organization, or system, including its own workforce; and (3) responding by putting this knowledge into practice” (SAMHSA, 2012, p 4).
Psychological First Aid
Building on the work of Everly (Everly & Lating, 2012), a group of practitioners and researchers formalized a protocol called Psychological First Aid (Brymer, et al., 2006, 2012). This program incorporated a growing consensus regarding the nature of resilience, the neurological impact of stress and trauma, and factors that maximize post-traumatic growth. It was designed for first responders, regardless of their role as medical, mental health, or citizen volunteers, as all persons serving the needs of survivors are providing a type of first aid necessary for long-term recovery.
The protocol consists of eight identified need themes of survivors, entitled Core Actions. Each of the Core Actions is accompanied by a description of the knowledge, skills, and dispositions required to enact it. The sponsors of the protocol, the National Child Traumatic Stress Network and the National Center for Post-Traumatic Stress Disorder, offer a guided tutorial in Psychological First Aid, and recommend that professional as well as citizen responders receive training in the protocol from an experienced trauma-informed trainer. See Figure 5.1 for a summary of the Core Actions, along with a link to access the online tutorial. This protocol is now the gold standard guiding all first responders, including educators responding to school-based traumatic events.
Psychological First Aid: Eight Core Actions
- Contact and Engagement: To [connect with survivors as] initiated by survivors, or to initiate [contact] in a non-intrusive, compassionate, and helpful manner.
- Safety and Comfort: To enhance immediate and ongoing safety, and provide physical and emotional comfort.
- Stabilization (if needed): To calm and orient emotionally overwhelmed or disoriented survivors [as appropriate for role and training].
- Information Gathering on Current Needs and Concerns: To identify immediate needs and concerns, gather additional information, and tailor Psychological First Aid interventions.
- Practical Assistance: To offer practical help to survivors in addressing immediate needs and concerns.
- Connection with Social Supports: To help establish brief or ongoing [contact] with primary support persons and other sources of support, including family members, friends, and community helping resources.
- Information on Coping: To provide information about stress reactions and coping to reduce distress and promote adaptive functioning [as designed by trauma-informed sources].
- Linkage with Collaborative Services: To link survivors with available services needed at the time or in the future.
At the core of Psychological First Aid is the provision of safety—making sure a survivor knows they are physically safe, their needs and distress are seen, and help is available to them, leading to a sense of emotional safety as precursor to beginning the work of recovery.
Psychological First Aid recognizes the benefits of connecting survivors with their community. As you dig deeper into the Core Actions, a responder is advised to recognize that they can serve the survivor best by connecting them with known, trusted others, such as the survivor’s immediate family and friends, as their relational community—their attachment base—has the greatest potential for activating their coping skills.
The Psychological First Aid protocol was created in response to the vast array of trauma responders who were misapplying good strategies or employing strategies that were doing more harm than good. We see this tendency continuing today, as many settings attempt to be trauma-informed without a grounding in the knowledge, skills, and dispositions prerequisite to exercising the perceptual, conceptual, and executive skills key to safe and effective implementation.
Trauma Informed Care
The Four Rs Of Trauma Informed Care
A program, organization, or system that is trauma informed:
Realizes the widespread impact of trauma and understand potential paths for recover;
Recognizes the signs and symptoms of trauma in clients, families, staff, and others involved with the system;
Responds by fully integrating knowledge about trauma into policies, procedures, and practices; and seeks to actively resist re-traumatization.
Resists re-traumatization of clients as well as staff.
Substance Abuse Mental Health Administration (SAMHSA, 2014)
Trauma-informed care (TIC): TIC is a strengths-based service delivery approach “that is grounded in an understanding of and responsiveness to the impact of trauma, that emphasizes physical, psychological, and emotional safety for both providers and survivors, and that creates opportunities for survivors to rebuild a sense of control and empowerment” (Hopper, Bassuk, & Olivet, 2010, p. 82). It also involves vigilance in anticipating and avoiding institutional processes and individual practices that are likely to re-traumatize individuals who already have histories of trauma, and it upholds the importance of consumer participation in the development, delivery, and evaluation of services.
Principles-of-Trauma-Informed-Care
The Tri-Phasic Model of Recovery
As early as 1886, Pierre Janet (Van Der Hart, Brown, & van der Kolk, 1989) identified that persons in a state of distress required professionals to envision a three-phase treatment process:
- First, help a distressed person establish an inner sense of safety and stabilization, given that the nature of their past or some current stressor is causing social, cognitive, and/or emotional dysregulation. This safety and stabilization phase requires professionals to recognize that the person seeking services needs to trust the provider and trust that they are not in immediate danger before they can dedicate energy to strengthening external and internal resources needed to increase their window of tolerance for distressing thoughts, feelings, and physical sensations.
- Once the person can self-stabilize, thereby increasing their capacity to tolerate and self-regulate when encountering distressing thoughts, feelings, and sensations, the person is then ready to engage in the emotionally stressful work of articulating the traumatic events causing the distress, and work through the meaning and impact of those events. The heart of this phase is what we now describe as memory integration work, in which we encounter and rework inner positive and negative neural networks. It is the working-through process that is the heart of therapy or recovery.
- Once the person is able to remember and mourn, hence integrate, these realities in a more conscious (aware) way, they can envision how they might want to let their history inform rather than stop their life. Moving forward with a renewed sense of purpose and meaning is now more possible.
This tri-phasic model comprised of (a) safety and stabilization, (b) remembrance and mourning, and (c) reintegration or re-engagement is a foundational concept guiding trauma recovery, whether working with children or adults, and regardless of treatment model (Baranowsky, Gentry, & Schultz, 2005; Herman, 1992; Shapiro, 2018).
Once again we see best practices supporting a universal principle that when we feel seen and valued, our anxiety circuits calm down, and we are more able to learn coping skills needed to tolerate anxiety and stress. And once we have gained mastery over our internal responses to current or past traumatizing events, we are in a place to learn new ways of thinking and responding to those realities.
Interventions Beyond the Initial Response to Trauma
A majority of this section is pulled from https://www.ncbi.nlm.nih.gov/books/NBK207184/. Please see this site for additional treatment strategies.
In the interest of increasing your overall familiarity with relevant approaches, the following sections review several traumatic stress treatment approaches that counselors will most likely encounter when collaborating with clinicians or agencies that specialize in trauma-specific services and treating traumatic stress.
Cognitive–behavioral therapies
Most PTSD models involve cognitive–behavioral therapy (CBT) that integrates cognitive and behavioral theories by incorporating two ideas: first, that cognitions (or thoughts) mediate between situational demands and one’s attempts to respond to them effectively, and second, that behavioral change influences acceptance of altered cognitions about oneself or a situation and establishment of newly learned cognitive–behavioral interaction patterns. In practice, CBT uses a wide range of coping strategies.
There are many different varieties of CBT. CBT originated in the 1970s (Beck, Rush, Shaw & Emery, 1979; Ellis & Harper, 1975) and has expanded since then to address various populations, including people who use substances, people who experience anxiety, people with PTSD or personality disorders, children and adolescents, individuals involved in the criminal justice system, and many others. CBT has also been expanded to include various techniques, coping skills, and approaches, such as dialectical behavior therapy (DBT; Linehan, 1993), Seeking Safety (Najavits, 2002a), and mindfulness (Segal, Williams, & Teasdale, 2002). Traditional CBT emphasizes symptom reduction or resolution, but recent CBT approaches have also emphasized the therapeutic relationship, a particularly important dynamic in trauma treatment ( Jackson, Nissenson, & Cloitre, 2009).
CBT has been applied to the treatment of trauma and has also been widely and effectively used in the treatment of substance use. A review of efficacy research on CBT for PTSD is provided by Rothbaum, Meadows, Resick, and Foy (2000). Najavits and colleagues (2009) and O’Donnell and Cook (2006) offer an overview of CBT therapies for treating PTSD and substance abuse. In addition, a free online training resource incorporating CBT for traumatized children within the community, Trauma-Focused CBT, is available from the Medical University of South Carolina (http://tfcbt.musc.edu/).
Cognitive processing therapy
Cognitive processing therapy (CPT) is a manualized 12-session treatment approach that can be administered in a group or individual setting (Resick & Schnicke, 1992, 1993). CPT was developed for rape survivors and combines elements of existing treatments for PTSD, specifically exposure therapy (see the “Exposure Therapy” section later in this chapter) and cognitive therapy. The exposure therapy component of treatment consists of clients writing a detailed account of their trauma, including thoughts, sensations, and emotions that were experienced during the event. The client then reads the narrative aloud during a session and at home. The cognitive therapy aspect of CPT uses six key PTSD themes identified by McCann and Pearlman (1990): safety, trust, power, control, esteem, and intimacy. The client is guided to identify cognitive distortions in these areas, such as maladaptive beliefs.
Results from randomized, placebo-controlled trials for the treatment of PTSD related to interpersonal violence (Resick, 2001; Resick, Nishith, Weaver, Astin, & Feuer, 2002) support the use of CPT. CPT and prolonged exposure therapy models are equally and highly positive in treating PTSD and depression in rape survivors; CPT is superior in reducing guilt (Nishith, Resick, & Griffin, 2002; Resick et al., 2002; Resick, Nishith, & Griffin, 2003). CPT has shown positive outcomes with refugees when administered in the refugees’ native language (Schulz, Marovic-Johnson, & Huber, 2006) and with veterans (Monson et al., 2006). However, CPT has not been studied with high-complexity populations such as individuals with substance dependence, homelessness, current domestic violence, serious and persistent mental illness, or suicidality. CPT requires a 3-day training plus consultation (Karlin et al., 2010). Resick and Schicke (1996) published a CPT treatment manual, Cognitive Processing Therapy for Rape Victims: A Treatment Manual.
Exposure therapy
Exposure therapy for PTSD asks clients to directly describe and explore trauma-related memories, objects, emotions, or places. Intense emotions are evoked (e.g., sadness, anxiety) but eventually decrease, desensitizing clients through repeated encounters with traumatic material. Careful monitoring of the pace and appropriateness of exposure-based interventions is necessary to prevent retraumatization (clients can become conditioned to fear the trauma-related material even more). Clients must have ample time to process their memories and integrate cognition and affect, so some sessions can last for 1.5 hours or more. For simple cases, exposure can work in as few as 9 sessions; more complex cases may require 20 or more sessions (Foa, Hembree, & Rothbaum, 2007). Various techniques can expose the client to traumatic material. Two of the more common methods are exposure through imagery and in vivo (“real life”) exposure.
The effectiveness of exposure therapy has been firmly established (Rothbaum et al., 2000); however, adverse reactions to exposure therapy have also been noted. Some individuals who have experienced trauma exhibit an exacerbation of symptoms during or following exposure treatments. Even so, the exacerbation may depend on counselor variables during administration. Practitioners of exposure therapy need comprehensive training to master its techniques (Karlin et al., 2010); a counselor unskilled in the methods of this treatment model can not only fail to help his or her clients, but also cause symptoms to worsen.
Exposure therapy is recommended as a first-line treatment option when the prominent trauma symptoms are intrusive thoughts, flashbacks, or trauma-related fears, panic, and avoidance. However, counselors should exercise caution when using exposure with clients who have not maintained stability in managing mental illness symptoms or abstinence from substance use disorders. Studies and routine use of exposure have consistently excluded high-complexity clients such as those with substance dependence, homelessness, current domestic violence, serious and persistent mental illness, or suicidality. The only trial of exposure therapy with a substance dependence sample found that it did not outperform standard substance abuse treatment on most variables (Mills et al., 2012).
Eye movement desensitization and reprocessing
EMDR (Shapiro, 2001) is one of the most widely used therapies for trauma and PTSD. The treatment protocols of EMDR have evolved into sophisticated paradigms requiring training and, preferably, clinical supervision. EMDR draws on a variety of theoretical frameworks, including psychoneurology, CBT, information processing, and nonverbal representation of traumatic memories. The goal of this therapy is to process the experiences that are causing problems and distress. It is an effective treatment for PTSD (Seidler & Wagner, 2006) and is accepted as an evidence-based practice by the U.S. Department of Veterans Affairs (VA), the Royal College of Psychiatrists, and the International Society for Traumatic Stress Studies (Najavits, 2007a); numerous reviews support its effectiveness (e.g., Mills et al., 2012). EMDR values the development of “resource installation” (calming procedures) and engages in exposure work to desensitize clients to traumatic material, using external tracking techniques across the visual field to assist in processing distressing material. Training in EMDR, available through the EMDR Institute, is required before counselors use this treatment. It is listed in SAMHSA’s NREPP (EMDR Network, 2012). Thus far, there is no study examining the use of EMDR with clients in substance abuse treatment. See Part 3 of this TIP, available online, to review empirical work on EMDR.
A Brief Description of EMDR Therapy
Treatment involves three main concentrations (past memories, present disturbances, future actions) and eight phases. Counselors may work with several phases in one session. Each phase is meant to be revisited either in every session or when appropriate (e.g., the closure process is meant to be conducted at the end of every session, in preparation for the next).
- Phase 1: History and Treatment Planning (1–2 sessions)
- Phase 2: Preparation
- Phase 3: Assessment and Reprocessing
- Phase 4: Desensitization
- Phase 5: Installation
- Phase 6: Body Scan
- Phase 7: Closure
- Phase 8: Reevaluation
Source: EMDR Network, 2012.
EMPOWER Model
In 2013, the Engage, Motivate, Protect, Organize, self- Worth, Educate, Respect (EMPOWER) Clinic for Survivors of Sex Trafficking and Sexual Violence was created to offer trauma- informed, long-term gynecologic and psychiatric care to survivors of sexual and gender-based violence in the New York City area. The EMPOWER Clinic recognizes that sexual and gender-based violence encompasses a wide range of acts, including rape and sexual assault, sex trafficking, child sexual abuse, intimate partner violence, and female genital cutting and responds inclusively to all survivors. There are numerous clinics throughout the U.S. that provide immediate physical care to survivors of sexual assault, just as there are practitioners who provide emotional support. However the EMPOWER Clinic is dedicated to both long-term medical and psychological care for survivors of sexual trauma, employing an evidenced-based, trauma informed approach (Ades, et al, 2019). With highly conscientious practices in response to the range of trauma response from sexual assault survivors, the EMPOWER Model provides a useful example for many other practitioner/clinic responses.
An example of reference points for health care providers within the EMPOWER Model.
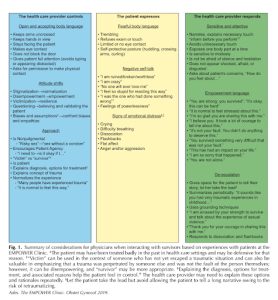
https://openoregon.pressbooks.pub/app/uploads/sites/216/2022/10/EMPOWER-Model.jpg
Conclusion
Issues of sexual assault are complex, varied and deeply impactful both personally and societally. This section sought to identify rates of sexual assault, intersectional challenges for survivors, as well as response and treatment modalities.
Importantly, this chapter has also shed light on the intersectional nature of sexual violence, recognizing that factors such as race, gender identity, and socioeconomic status can significantly influence both the experience of trauma and access to care. The discussion of human trafficking further emphasizes the complexity of these issues and the need for comprehensive, yet nuanced approaches to prevention and intervention.
As we move forward, it’s crucial to continue developing and implementing trauma-informed practices across various sectors, from healthcare to law enforcement and education. By increasing awareness, challenging societal norms that perpetuate violence, and providing compassionate, effective care to survivors, we can work towards a society that not only responds to sexual violence but actively works to prevent it.
The journey of healing from sexual trauma is unique for each survivor, but with continued research, improved practices, and a commitment to creating a culture of consent and respect, we can hope to create a world where fewer individuals experience such trauma, and those who do receive the support and care they need to heal and thrive.
Reflection Questions
- We discuss/define the concept of “rape culture.” How might societal attitudes and norms contribute to the perpetuation of sexual violence? Can you think of any examples in media, law, or everyday life that could be seen as reinforcing rape culture?
- The reading mentions various risk and protective factors for sexual violence perpetration. How might understanding these factors help in developing prevention strategies? What role could education, community programs, or policy changes play in addressing these factors?
- We go over several trauma-informed approaches to care and therapy for survivors of sexual violence. How do these approaches differ from traditional therapeutic methods? Why might trauma-informed care be particularly important for survivors of sexual violence?
- Consider the section on human trafficking. How does the chapter distinguish between sex work and human trafficking? What challenges might arise in identifying and supporting victims of sex trafficking?
- The EMPOWER model is presented as an approach to providing care for survivors of sexual violence. How does this model address the complex needs of survivors? Can you think of ways this approach could be applied or adapted in other healthcare or support settings?
Licenses & Attributions
Centers for Disease Control and Prevention. Sexual Violence. Creative Commons Attribution 3.0 License.
Center for Substance Abuse Treatment (US). Trauma-Informed Care in Behavioral Health Services. Rockville (MD): Substance Abuse and Mental Health Services Administration (US); 2014. (Treatment Improvement Protocol (TIP) Series, No. 57.) Chapter 6, Trauma-Specific Services. Available from: https://www.ncbi.nlm.nih.gov/books/NBK207184/ Adaptations: Reformatted. Added learning objectives. Modified content for language, application to subject and cohesion. Updated sources. All Rights Reserved
Katz, J. (2012). Violence against women–it’s a men’s issue. TED. https://www.ted.com/talks/jackson_katz_violence_against_women_it_s_a_men_s_issue?referrer=playlist-the_conversation_around_sexual_assault&autoplay=true
Psych Hub (2021). Cognitive processing therapy. https://www.youtube.com/watch?v=_8a-dVIHumE License: Psych Hub, LLC. All Rights Reserved.
SciShow Psych (2018, May 24). Can moving your eyes re-code your memories? https://www.youtube.com/watch?v=659ySOKyoiU. License: All Rights Reserved. License Terms: Standard YouTube license.
References
Ades, V., Wu, S. X., Rabinowitz, E., Bach, S. C., Goddard, B., Ayala, S. P., & Greene, J. (2019). An integrated, trauma-informed care model for female survivors of sexual violence: the Engage, Motivate, Protect, Organize, Self-Worth, Educate, Respect (EMPOWER) Clinic. Obstetrics & Gynecology, 133(4), 803-809.
Alexander, C. S. (2020). Sorry (not sorry): Decoding #MeToo defenses. Texas Law Review, 99(2), 341–388.
Basile, K. C., Smith, S. G., Breiding, M. J., Black, M. C., & Mahendra, R. R. (2014). Sexual violence surveillance: Uniform definitions and recommended data elements, version 2.0. Atlanta (GA): National Center for Injury Prevention. https://www.cdc.gov/violenceprevention/pdf/sv_surveillance_definitionsl-2009-a.pdf.
Benner, J. (2018). Implementing trauma-informed care in all spaces. Family & Intimate Partner Violence Quarterly, 10(4). https://eds.a.ebscohost.com/eds/pdfviewer/pdfviewer?vid=1&sid=aa4fb21b-8a80-4b90-8d8e-84e0a5d8a78a%40sdc-v-sessmgr03
Berardi, A. A. & Morton, B. M. (2019). Trauma informed school practices. https://open.umn.edu/opentextbooks/textbooks/718
Center for Disease Control and Prevention. (2020, January). Sexual violence. https://www.cdc.gov/violenceprevention/sexualviolence/index.html. National Center for Injury Prevention and Control, Division of Violence Prevention.
Center for Substance Abuse Treatment (US). (2014). Trauma-informed care in behavioral health services. Substance Abuse and Mental Health Services Administration (US). https://www.ncbi.nlm.nih.gov/books/NBK207201/
Cuevas, K. M., Balbo, J., Duval, K., & Beverly, E. A. (2018). Neurobiology of sexual assault and osteopathic considerations for trauma-informed care and practice. Journal of the American Osteopathic Association, 118(2), e2-e10. https://jaoa.org/aoa/content_public/journal/jaoa/936734/e2.pdf
Evans, DSW, H. R. (2019). From the Voices of Domestic Sex Trafficking Survivors: Experiences of Complex Trauma & Posttraumatic Growth. Retrieved from https://repository.upenn.edu/cgi/viewcontent.cgi?article=1131&context=edissertations_sp2
Kessler, A. M., Kennair, L. E. O., Grøntvedt, T. V., Bjørkheim, I., Drejer, I., & Bendixen, M. (2020). The effect of prototypical #MeToo features on the perception of social-sexual behavior as sexual harassment. Sexuality & Culture, 24(5), 1271–1291. https://doi-org.libproxy.pcc.edu/10.1007/s12119-019-09675-7
Klement, K. R., Sagarin, B. J., & Lee, E. M. (2017). Participating in a culture of consent may be associated with lower rape-supportive beliefs. The Journal of Sex Research, 54(1), 130–134. Doi: 10.1080/00224499.2016.1168353
Korn, D. L. (2009). EMDR and the treatment of complex PTSD: A review. Journal of EMDR Practice and Research, 3(4), 264-278. https://connect.springerpub.com/content/sgremdr/3/4/264.full.pdf
Lewis, K. R., Robillard, A., Billings, D., & White, K. (2019). Differential perceptions of a hypothetical sexual assault survivor based on race and ethnicity: Exploring victim responsibility, trauma, and need for social support. Journal of American college health, 67(4), 308-317. https://pubmed.ncbi.nlm.nih.gov/29952734/
McQuaid, J. (2020). Understanding the psychological effects of sex trafficking to inform service delivery. Forced Migration Review, (64), 42-44. https://search.proquest.com/openview/adc05e0721e6114f5269b2a6cb5da99f/1?cbl=55113&pq-origsite=gscholar
National Domestic Violence Hotline. (2019, November). A deeper look into gaslighting. https://www.thehotline.org/2019/11/22/a-deeper-look-into-gaslighting/
Rape, Abuse, & Incest National Network [RAINN]. (2021). National sexual assault hotline. https://www.rainn.org/about-national-sexual-assault-telephone-hotline
Richmond, K., Geiger, E., & Reed, C. (2013). The personal is political: A feminist and trauma-informed therapeutic approach to working with a survivor of sexual assault. Clinical Case Studies, 12(6), 443-456. https://journals.sagepub.com/doi/pdf/10.1177/1534650113500563
Van der Hart, O., Brown, P., & Van der Kolk, B. A. (1989). Pierre Janet’s treatment of post-traumatic stress. Journal of traumatic stress, 2(4), 379-395.
Van der Kolk, B. A. (2014). The body keeps the score: Brain, mind, and body in the healing of trauma. Viking.
Vikman, E. (2005). Ancient origins: Sexual violence in warfare, Part I. Anthropology & Medicine, 12(1), 21–31. https://doi-org.libproxy.pcc.edu/10.1080/13648470500049826

